Summer Scare: Flesh-Eating Bacteria Claims Six Lives on East Coast, Meningococcal Disease Outbreak in Virginia Sparks Concern


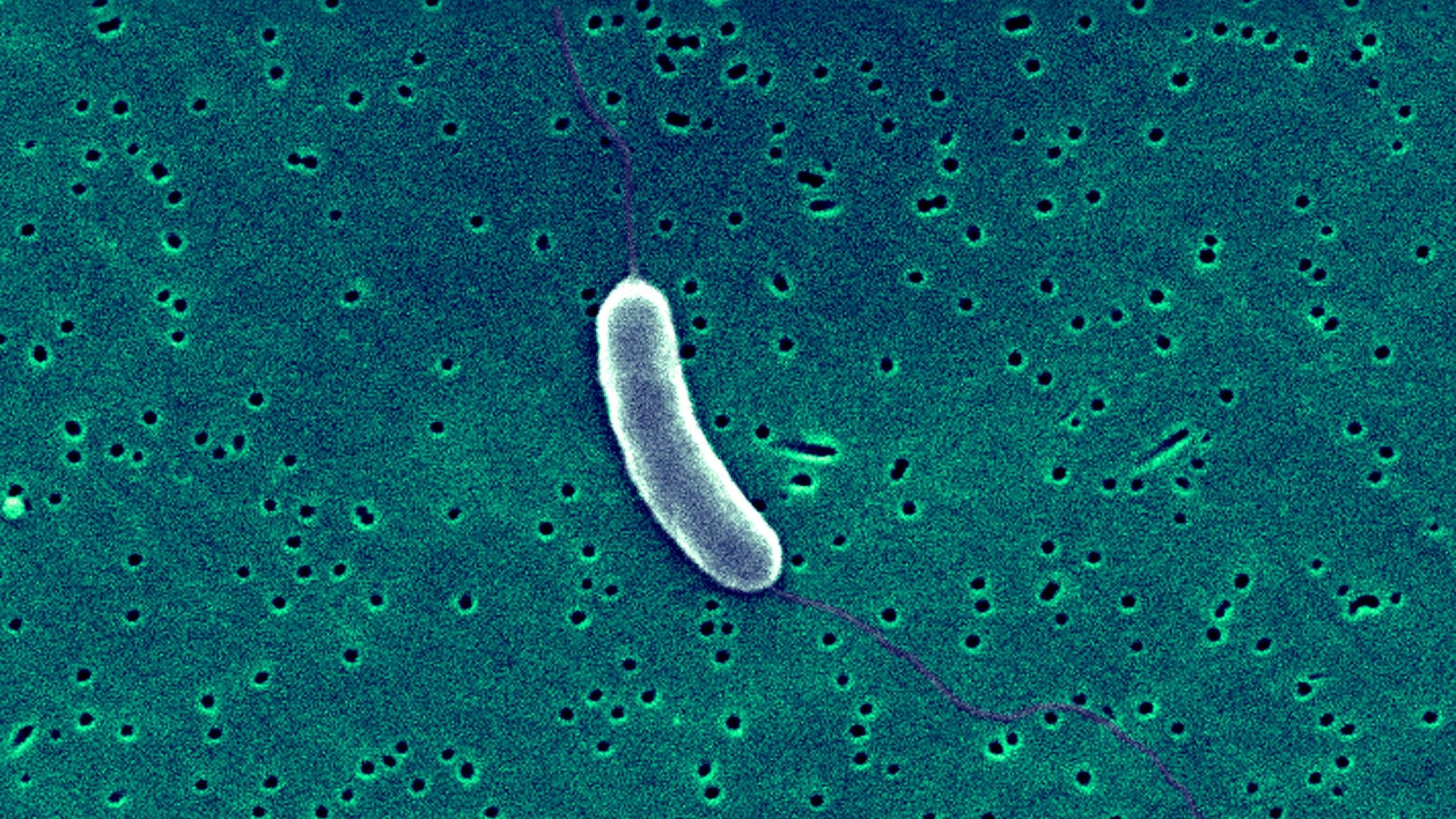 Warming Waters Bring ‘Flesh-Eating’ Bacteria Deaths, Virginia Grapples with Meningococcal Outbreak
Warming Waters Bring ‘Flesh-Eating’ Bacteria Deaths, Virginia Grapples with Meningococcal Outbreak
As the end of summer heats up, a chilling health alert has struck the East Coast of the United States.
At least six people have tragically lost their lives after contracting a “flesh-eating” bacteria in the warm coastal waters.
Health officials confirm that two individuals in Connecticut, one in New York, and three in North Carolina fell victim to Vibrio vulnificus, a potentially deadly bacterium, during July and August.
While the Gulf states typically witness a handful of such cases, it’s a rare occurrence for these deaths to spike on the East Coast.
Responding to this alarming trend, the Centers for Disease Control and Prevention (CDC) has issued a health advisory, urging doctors, laboratories, and public health departments to be vigilant for these infections.
Dr. Rita Colwell, a microbiologist and marine expert, warns, “The sky is not falling, but be careful, pay attention, and take it seriously if you have an infection and get it treated.”
Understanding the Threat: Vibrio Vulnificus
Vibrio bacteria are responsible for approximately 80,000 illnesses in the United States each year.
Among them, Vibrio vulnificus stands out as a potential life-threatening culprit.
The CDC reports between 150 and 200 infections annually, with an alarming one in five individuals succumbing to the infection, often within just a day or two of becoming ill.
These bacteria are naturally present in saltwater and brackish waters, with their prevalence peaking during the summer months, from May to October.
Dr. Antarpreet Jutla, an environmental engineering science professor, explains, “Most often than not, this bacterium is going to have a coastal origin, meaning that somebody would visit coastal waters for recreation, they may have a wound or exposed skin.”
Moreover, consuming raw or undercooked shellfish, particularly oysters from coastal waters, can heighten the risk of infection.
Symptoms of Vibrio vulnificus infection range from fever, nausea, vomiting, and stomach cramps to watery diarrhea.
For those with a bloodstream infection, symptoms escalate to include fever, chills, low blood pressure, and blistering skin lesions.
Wound infections can lead to necrotizing fasciitis, a condition where the flesh around an open wound dies, sometimes necessitating limb amputation.
Root Causes of Infection
Many of the infections in Connecticut, New York, and North Carolina were linked to open wounds exposed to coastal waters, while others were traced back to the consumption of raw or undercooked seafood.
Some infections, however, had unclear origins.
To minimize the risk, health officials advise individuals with open wounds to avoid saltwater and brackish water.
In case of contact, thoroughly clean the wound with clean, running water and soap. Additionally, steer clear of raw shellfish.
Tessa Getchis, an extension educator, emphasizes, “If you got cut and it’s healed over, that’s not a problem. If it’s an open wound, they want to wait until that wound is closed.”
Future Concerns and Environmental Factors
With coastal populations growing and warmer temperatures prolonging the warm season, this issue could become more prevalent in the future.
Recent hurricane events, like Hurricane Idalia, have heightened concerns. Floodwaters and storm surges provide opportunities for Vibrio vulnificus infection.
Dr. Jutla advises caution, stating, “If I were in that region, I would not wander around in flooded waters… I would be very careful in going to sea water coastal waters.”
Meningococcal Disease Outbreak in Virginia Raises Alarms
In a separate health crisis, Virginia is grappling with an outbreak of rare but severe meningococcal disease.
Since June 2022, the state has reported 27 cases, three times higher than the expected number during this period.
Tragically, five individuals have succumbed to complications related to the disease.
Most of the patients affected by this outbreak are Black or African American adults aged 30 to 60.
Although no common risk factor has been identified, genetic sequencing suggests a shared origin of the bacteria responsible for the outbreak.
Meningococcal disease, caused by Neisseria meningitidis, is transmitted through contact with an infected person’s saliva or spit, such as through coughing, kissing, sharing items, or close proximity to an infected person.
The disease can lead to severe conditions like meningitis (inflammation of the brain and spinal cord lining) and septicemia (bloodstream infection).
Symptoms include headache, fever, stiff neck, nausea, vomiting, sensitivity to light, and a distinctive dark purple rash if the disease enters the bloodstream.
Early diagnosis is critical, and antibiotics can effectively treat meningococcal disease.
However, prompt treatment is essential to reduce the risk of complications, which can include deafness, limb loss, brain damage, and nervous system problems.
The Virginia Department of Health recommends several preventive measures, including not sharing personal items, practicing good hand hygiene, avoiding contact with sick individuals, and seeking immediate care if experiencing meningococcal disease symptoms.
As these two health crises unfold, vigilance, prevention, and education are essential to safeguard public health on the East Coast and beyond.
Read the original story here:
ABC News

